“Autonomous Driving” for Medical AI: Will Surgery as a Profession Face an Impact?

Interviewee: Dr. Qiang Zhang
Virtual Editor: Daniel Ho (Asian Venous Academy · Hong Kong)
Background: In July 2025, a research team from Johns Hopkins University released a breakthrough study: their AI-driven robot, SRT-H, successfully and independently performed key steps of a laparoscopic cholecystectomy without human intervention, sent shockwaves through the global medical community.
The Redefinition of Professional Boundaries
Daniel Ho: Dr. Zhang, in July 2025, the SRT-H surgical robot completed key steps of a gallbladder removal autonomously. The initial reaction among surgeons was one of shock. How do you perceive the true significance of this milestone?
Dr. Zhang: In my view, this isn’t just news about a robot’s “technical success”; it is a signal that professional boundaries are being redefined. For over a century, a surgeon’s core competitiveness has been built on three pillars: manual stability, path selection based on accumulated experience, and real-time response to complications.
What systems like SRT-H truly disrupt is not the “ability to cut,” but rather the ability to consistently, stably, and tirelessly replicate the optimal surgical path within standardized scenarios. It signifies that the era of surgery centered on “the hand” has begun to shift.
The Surgeon’s New Position
Daniel Ho: Many surgeons are asking a blunt question: If standard procedures can be completed by AI, where is our place in the operating room?
Dr. Zhang: We must deconstruct this. AI’s advantage will always lie in standardization, reproducibility, and high-frequency operations. Conversely, the truly irreplaceable qualities of a surgeon involve three domains:
-
Clinical Judgment: Deciding what not to do.
-
Personalization: Understanding why a specific patient deviates from the standard model.
-
Accountability: Assuming responsibility amidst uncertainty.
The surgeon of the future will not disappear, but their role will migrate from “primary executor” to “system supervisor,” “risk architect,” and “final arbiter of medical logic.” This is not a demotion; it is an upward shift in the center of gravity for the profession.
Beyond the Scalpel: A Systemic Shift
Daniel Ho: If we look beyond “robotic surgery” to broader technological evolutions—pharmacology, exercise prescriptions, interventional techniques, and non-invasive devices—where do you think the real impact on surgery originates?
Dr. Zhang: Excision and destruction are no longer the only answers. Historically, surgery solved problems by identifying structural abnormalities and removing or replacing them. Today, however, more technologies are bypassing “destruction” altogether. Pharmacology is reshaping long-term disease progression; exercise prescriptions are altering mechanical loads; non-invasive devices are allowing for earlier intervention; and AI is restructuring the logic of assessment and decision-making.
Surgery is no longer the final destination; it has become one option within a system. If a surgeon still defines themselves solely as “someone who performs operations,” they will indeed be marginalized by this era.
The Case of Venous Surgery and CHIVA
Daniel Ho: This seems particularly evident in the field of venous surgery, doesn’t it?
Dr. Zhang: Exactly. Venous disease is a prime example because it was never just a matter of “cutting it out.” It is a hemodynamic issue. For decades, we were accustomed to using stripping, closure, or ablation to treat varicose veins—essentially using “structural destruction” to address “functional imbalance.”
As AI enhances our ability to analyze ultrasound, simulate blood flow, and predict long-term pathways, a philosophy closer to physiological logic is re-emerging: CHIVA.
Daniel Ho: You have often emphasized the “natural synergy” between CHIVA and AI. Could you elaborate?
Dr. Zhang: The core of CHIVA is not a specific surgical trick, but a decision-making philosophy: do not rush to eliminate the vessel. Instead, prioritize identifying the source of reflux and use minimal intervention to reconstruct pressure and flow. This is precisely what AI excels at: multi-variable analysis, path prediction, and outcome simulation.
The Role of the Asian Venous Academy
Daniel Ho: Is this part of the vision behind the establishment of the Asian Venous Academy in Hong Kong?
Dr. Zhang: You could say that, but the significance extends beyond the venous field. The Academy was born at a critical inflection point—where surgery moves from “technology-led” to “system-led.” Hong Kong’s value lies in its position at the intersection of international medical discourse. The Asian Venous Academy is not just an institution for “promoting techniques”; it is a platform for discussing the future logic of medicine.
Daniel Ho: If you could say one thing to your surgical colleagues, what would it be?
Dr. Zhang: I would say that AI is not the end of surgery; it is the catalyst for the transformation of the “pure operator.” In the future, what matters most is not whether you can still perform the manipulation, but whether you understand how a disease is shaped over time, how an intervention alters the system, and when the best choice is “to do nothing.” This is the hallmark of surgery reaching its maturity.
Daniel Ho: Thank you, Dr. Zhang.
Closing Thoughts: When AI begins to perform surgery independently, the true test is not for the machine, but for the surgeon’s willingness to embrace a higher-dimensional definition of their profession. At this pivotal moment, the Asian Venous Academy seeks to provide a long-term, open, and serious space for this vital discussion.
“Autonomous Driving” for Medical AI: Will Surgery as a Profession Face an Impact?

Interviewee: Dr. Qiang Zhang
Virtual Editor: Daniel Ho (Asian Venous Academy · Hong Kong)
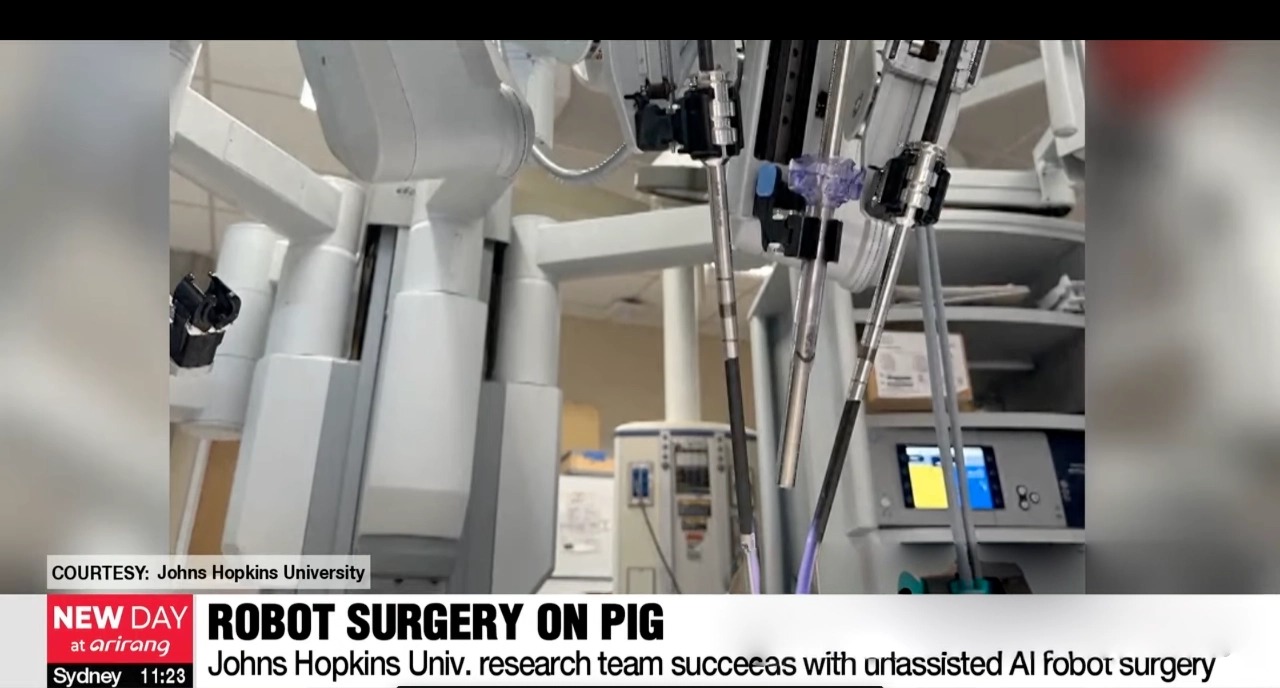
Background: In July 2025, a research team from Johns Hopkins University released a breakthrough study: their AI-driven robot, SRT-H, successfully and independently performed key steps of a laparoscopic cholecystectomy without human intervention, sent shockwaves through the global medical community.
The Redefinition of Professional Boundaries
Daniel Ho: Dr. Zhang, in July 2025, the SRT-H surgical robot completed key steps of a gallbladder removal autonomously. The initial reaction among surgeons was one of shock. How do you perceive the true significance of this milestone?
Dr. Zhang: In my view, this isn’t just news about a robot’s “technical success”; it is a signal that professional boundaries are being redefined. For over a century, a surgeon’s core competitiveness has been built on three pillars: manual stability, path selection based on accumulated experience, and real-time response to complications.
What systems like SRT-H truly disrupt is not the “ability to cut,” but rather the ability to consistently, stably, and tirelessly replicate the optimal surgical path within standardized scenarios. It signifies that the era of surgery centered on “the hand” has begun to shift.
The Surgeon’s New Position
Daniel Ho: Many surgeons are asking a blunt question: If standard procedures can be completed by AI, where is our place in the operating room?
Dr. Zhang: We must deconstruct this. AI’s advantage will always lie in standardization, reproducibility, and high-frequency operations. Conversely, the truly irreplaceable qualities of a surgeon involve three domains:
-
Clinical Judgment: Deciding what not to do.
-
Personalization: Understanding why a specific patient deviates from the standard model.
-
Accountability: Assuming responsibility amidst uncertainty.
The surgeon of the future will not disappear, but their role will migrate from “primary executor” to “system supervisor,” “risk architect,” and “final arbiter of medical logic.” This is not a demotion; it is an upward shift in the center of gravity for the profession.
Beyond the Scalpel: A Systemic Shift
Daniel Ho: If we look beyond “robotic surgery” to broader technological evolutions—pharmacology, exercise prescriptions, interventional techniques, and non-invasive devices—where do you think the real impact on surgery originates?
Dr. Zhang: Excision and destruction are no longer the only answers. Historically, surgery solved problems by identifying structural abnormalities and removing or replacing them. Today, however, more technologies are bypassing “destruction” altogether. Pharmacology is reshaping long-term disease progression; exercise prescriptions are altering mechanical loads; non-invasive devices are allowing for earlier intervention; and AI is restructuring the logic of assessment and decision-making.
Surgery is no longer the final destination; it has become one option within a system. If a surgeon still defines themselves solely as “someone who performs operations,” they will indeed be marginalized by this era.
The Case of Venous Surgery and CHIVA
Daniel Ho: This seems particularly evident in the field of venous surgery, doesn’t it?
Dr. Zhang: Exactly. Venous disease is a prime example because it was never just a matter of “cutting it out.” It is a hemodynamic issue. For decades, we were accustomed to using stripping, closure, or ablation to treat varicose veins—essentially using “structural destruction” to address “functional imbalance.”
As AI enhances our ability to analyze ultrasound, simulate blood flow, and predict long-term pathways, a philosophy closer to physiological logic is re-emerging: CHIVA.
Daniel Ho: You have often emphasized the “natural synergy” between CHIVA and AI. Could you elaborate?
Dr. Zhang: The core of CHIVA is not a specific surgical trick, but a decision-making philosophy: do not rush to eliminate the vessel. Instead, prioritize identifying the source of reflux and use minimal intervention to reconstruct pressure and flow. This is precisely what AI excels at: multi-variable analysis, path prediction, and outcome simulation.
The Role of the Asian Venous Academy
Daniel Ho: Is this part of the vision behind the establishment of the Asian Venous Academy in Hong Kong?
Dr. Zhang: You could say that, but the significance extends beyond the venous field. The Academy was born at a critical inflection point—where surgery moves from “technology-led” to “system-led.” Hong Kong’s value lies in its position at the intersection of international medical discourse. The Asian Venous Academy is not just an institution for “promoting techniques”; it is a platform for discussing the future logic of medicine.
Daniel Ho: If you could say one thing to your surgical colleagues, what would it be?
Dr. Zhang: I would say that AI is not the end of surgery; it is the catalyst for the transformation of the “pure operator.” In the future, what matters most is not whether you can still perform the manipulation, but whether you understand how a disease is shaped over time, how an intervention alters the system, and when the best choice is “to do nothing.” This is the hallmark of surgery reaching its maturity.
Daniel Ho: Thank you, Dr. Zhang.
Closing Thoughts: When AI begins to perform surgery independently, the true test is not for the machine, but for the surgeon’s willingness to embrace a higher-dimensional definition of their profession. At this pivotal moment, the Asian Venous Academy seeks to provide a long-term, open, and serious space for this vital discussion.